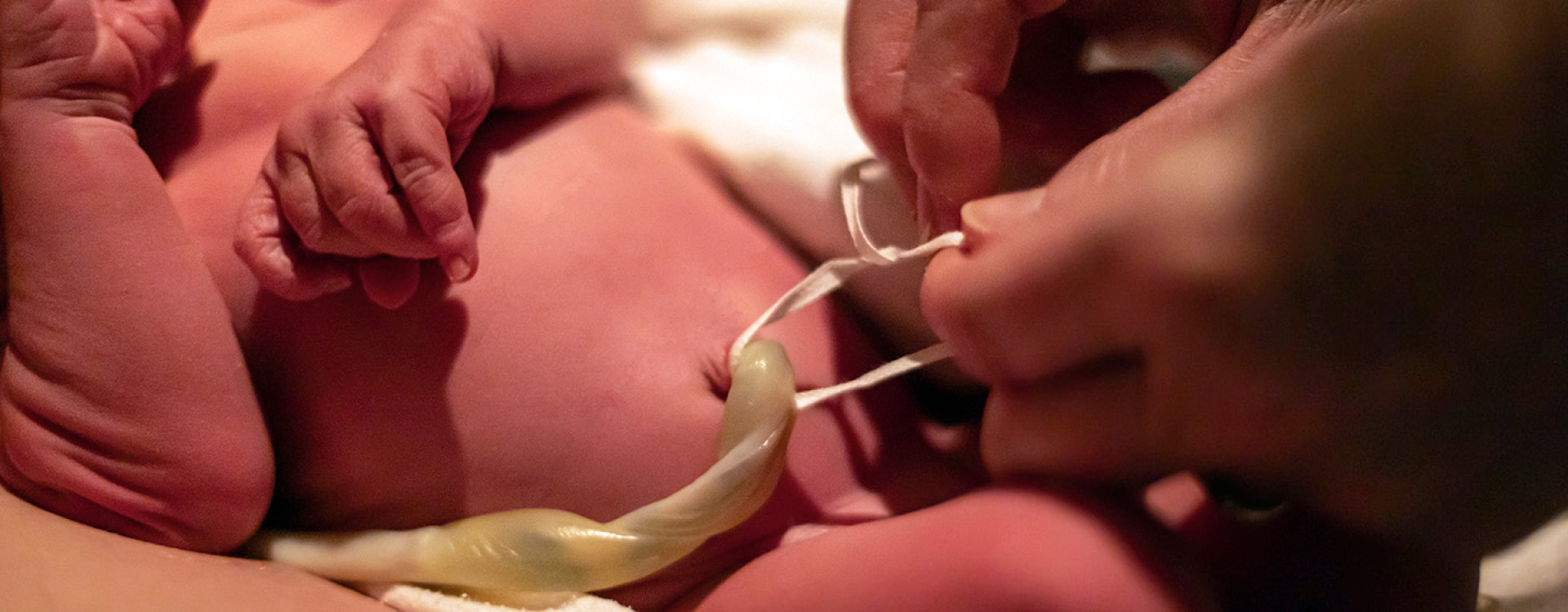
The question of when to clamp the umbilical cord after the infant has arrived has been debated for centuries and continues to be studied.
The medical community believes that term and preterm infants, delivered vaginally and by Cesarean, can benefit from the placental transfusion delayed cord clamping provides. But it’s not the standard of care for some hospitals.
Here’s what delayed cord clamping is, why experts recommend it, and why you should ask your care provider about it.
What Is Delayed Cord Clamping?
Delayed cord clamping means waiting for a period time before clamping and cutting the umbilical cord after birth. This allows more blood to flow from the placenta to the newborn.
At term, about a third of the fetus’s blood supply lives in the placenta. The intense uterine contractions of labor and delivery start to move this blood from placenta to newborn, but that process doesn't stop the minute the infant emerges from the womb — it can continue for 1-3 minutes just after birth, delivering more blood to the newborn.
Benefits of Delayed Cord Clamping
Experts believe that both term and preterm infants benefit from delayed cord clamping right after birth, in their first few months of life, and even beyond their first year. Here are a few of the benefits:
- Iron deficiency during infancy and childhood is linked to impaired cognitive, motor, and behavioral development that may be irreversible, according to ACOG (American College of Obstetricians and Gynecologists). The additional blood delayed cord clamping supplies provides iron to support the infant’s brain growth and development in their first few months, and may offset the potential for complications in their first year [*].
- According to a study by the American Academy of Pediatrics, delayed cord clamping may offer a more physiologic transition because it provides time for the infant to aerate the lungs and increase pulmonary blood flow before venous return from the placental circulation is lost. They note that previous studies have shown harm when clamping occurred before spontaneous respirations [*].
- The benefits are particularly pronounced with preterm infants with very low birth weight, and especially, male pre-term infants. One study found a significantly reduced incidence of hemorrhage inside the brain and late-onset sepsis among preterm and low birth weight infants who had delayed cord clamping performed, especially the male infants [*].
- Preterm infants undergoing delayed cord clamping have less need for blood transfusion and are less likely to have necrotizing enterocolitis, a life-threatening deterioration of the intestine. Some studies show improved hospital mortality outcomes as well.
- Term and preterm infants have shown immune system and other benefits from the added volume of red blood cells and stem cells provided by delayed cord clamping.
Risks of Delayed Cord Clamping
Over centuries, different risks have been associated with delayed cord clamping, but most have been proven irrelevant, statistically insignificant, or incorrect. These include conditions such as polycythemia (having a high concentration of red blood cells that makes blood thicker), hyperbilirubinemia (an overabundance of bilirubin in baby’s blood, typically treated with light therapy), and respiratory distress. The most recent studies find no real statistical difference among infants who had delayed cord clamping performed and those who did not for these conditions, and moreover, that the benefits of delayed cord clamping in the long and short term justify its practice.
Regarding the mother, delayed cord clamping is also not associated with an increased risk of postpartum hemorrhage, increased blood loss at delivery, or the need for postpartum transfusion. In other words, the blood that’s in the placenta is there for the baby and the mother is going to give it to the baby or expel it.
That said, there are some situations where other risks to the mother or child may mean that delayed cord clamping cannot be performed:
- If the mother is hemorrhaging and in need of urgent medical treatment.
- If there is an issue with the placenta or its position in the uterus that endangers the mother.
- If the cord itself is bleeding in a way that would compromise the transfer of blood.
- If the baby requires resuscitation or is categorized as “non-vigorous,” i.e., limp, pale, and with minimal breathing.
Cord Milking vs. Delayed Cord Clamping
Cord milking, which can be done in 15-20 seconds, may offer comparable results to delayed cord clamping in term and late preterm infants. A 2019 study found no difference in blood volume between infants undergoing cord milking and those undergoing delayed cord clamping among women who had vaginal births [*].
However, there are some risks associated with cord milking when used with early preterm infants whose vascular systems are fragile. The rapid infusion of blood from milking may cause intraventricular hemorrhage.
Also, it is highly unlikely that cord blood collection for cord blood banking can occur with cord milking. However, cord tissue (and cord tissue stem cells) can still be saved when cord milking is performed. It is always best to discuss what is most appropriate should your child be born preterm or otherwise with your care provider.
Expert Recommendations
Interestingly enough, delayed cord clamping was the standard of care until the 1950s, when a series of blood volume studies and the introduction of active management of the third stage of labor argued for immediate clamping.
In the last decade, the pendulum has swung back to favor delayed cord clamping for all births, delaying for 30-60 seconds [*]:
- The American Academy of Pediatrics recommends delayed cord clamping for at least 30-60 seconds after birth.
- The World Health Organization recommends that the umbilical cord not be clamped earlier than 1 minute after birth.
- The American College of Obstetricians and Gynecologists (ACOG) recommends delayed cord clamping for 30-60 seconds after birth [*].
Why Don’t All Hospitals Practice Delayed Cord Clamping Routinely?
A 2021 study noted that about half of U.S. hospitals perform delayed cord clamping as the standard of care where indicated. Why that number isn’t higher, given that the practice is safe, effective, and endorsed by virtually every regulating medical organization with a stake in fetal outcomes, is a contradiction that is hard to get your head around [*].
Delayed cord clamping is an ancient practice. As early as 1773, maternity doctors recognized that delayed cord clamping would benefit neonatal transition [*].
The practice of immediate clamping seems to have started in earnest in the 1940s to prevent maternal antibodies from entering the neonate in response to a certain blood disease, but by 1960, a new drug made this issue irrelevant. Virginia Apgar, namesake of the Apgar score, may also have had a role in subtly advocating against delayed cord clamping in writings published in the 1950s.
The justifications and purported benefits of early cord clamping have, with medical advances and research, frequently been proven irrelevant. Some argue that lack of knowledge, the strong influence of tradition, or the rise in surgically assisted births may be to blame [*].
Others claim it is fear of consequences for the ill or weak infant, and a lack of understanding as to how to implement delayed cord clamping in these scenarios. Roughly 10-15% of babies born each year will need some sort of resuscitation at birth. These infants could benefit from continued placental gas exchange as well as the blood delayed cord clamping provides. Studies comparing ventilation during delayed cord clamping to delayed cord clamping alone showed no difference in the average time it took to establish a breath, delivery room interventions, or early hemodynamics [*].
Delayed Cord Clamping FAQ
How long should delayed cord clamping last?
Most professional associations recommend 30-60 seconds. 80% of the blood in the placenta at birth is believed to flow to the infant in the first minute, so if you’re looking to save cord blood for banking, 30-60 seconds is what is recommended.
Is delayed cord clamping safe?
Yes. Physiologic-based cord clamping does not increase the risk of developing tachypnea (rapid breathing), clinical jaundice, or symptomatic polycythemia, according to the ACNM’s 2021 position paper on delayed cord clamping and cord milking [*]. Note that jaundice in newborns is very common. Up to 60% of full-term babies, and as many as 80% of preterm babies, develop jaundice during their first week of life. It goes away by itself or may be treated with light therapy [*].
Are there any maternal risks to delayed cord clamping?
No, when delayed cord clamping is safe to perform, it does not increase blood loss or lead to adverse effects.
Should I add delayed cord clamping to my birth plan?
It is worth a discussion with your healthcare provider to see if delayed cord clamping is ideal for your delivery. If you are saving your baby’s cord blood, please know that the longer the delay, the lower the volume of cord blood there will be for collection. That said, delaying for the recommended time of 30-60 seconds after birth will typically still yield a nice volume cord blood collection.
Is delayed cord clamping possible with c-section?
Yes, but women having a c-section, and especially preterm, may have urgencies that need prioritizing in the delivery room. Your doctor may need to make the final call. Also, cord blood collection is possible with a c-section and occurs very often.
Can you do delayed cord clamping and cord blood banking?
Yes! Whether you deliver vaginally or have a c-section, you can have your cake and eat it too because delayed cord clamping and cord blood banking are compatible. The first priority will always be to get the placental blood and stem cells to the infant at birth, but generally speaking, 30-60 seconds of delayed clamping will allow the benefits to accrue to the newborn and also allow for enough cord blood to be collected. Cord tissue collection and storage is not affected at all by delayed cord clamping or milking [*].
How much blood does the baby get with delayed cord clamping?
This depends on the size of the infant, whether it is term or preterm, the delivery type (vaginal or c-section, since labor contractions help infuse the placental blood to the infant), and how long the delayed cord clamping lasts.
About a third of the baby’s blood lives in the placenta at term. About 80% of that blood is believed to move to the infant in the first minute of delayed cord clamping.
The Bottom Line
Delayed cord clamping is safe, effective and has proven benefits for term and preterm infants that can positively impact them for a lifetime. Talk to your maternity provider about delayed cord clamping to ensure that your child comes into the world with all the resources they need and deserve.
Helping Baby at Birth and Beyond
Combining delayed cord clamping with cord banking offers another layer of protection for your family. Because the volume of cord blood is decreased by delayed cord clamping, it’s important to choose a cord blood bank that has processes designed maximize stem cell recovery.
MiracleCord’s TimeCritical® Processing combined with our lab’s AXPII® systems, is optimized to recover more viable stem cells. Request an Info Kit to learn more about our state-of-the-art processes, and why to choose MiracleCord.
DISCLAIMER: THE INFORMATION ON THIS WEBSITE IS NOT INTENDED TO BE USED AS MEDICAL ADVICE.The materials and information contained on the MiracleCord website is provided for educational and informational purposes only, and is not intended to, and does not constitute, medical or other health advice or diagnosis, and should not be used as such. You should not use this information to diagnose or treat a health problem or disease. If you are seeking personal medical advice, you should consult with a licensed physician. Always consult with a qualified health care provider regarding a medical condition.