Coning during pregnancy and post-partum is an underreported, undertreated condition that can lead to serious health problems. Learn how to recognize it and what to do about it before, during and after your pregnancy.
What Is Coning?
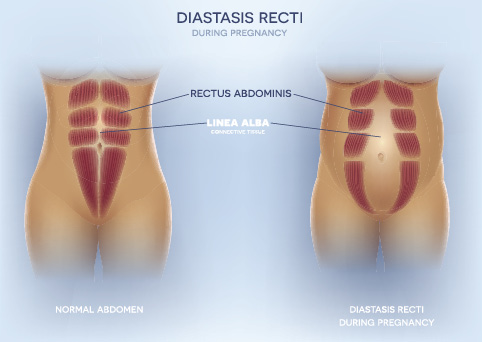
Coning is the common term for a linear protrusion down the midline of the abdomen which may also indicate a medical condition known as abdominal diastasis or diastasis recti (DR). It occurs when the connective tissue in the center of your abdomen (the linea alba) thins and tears away from your six-pack — the rectus abdominis muscle. This muscle covers the front surface of the belly area.
The normal width of the linea alba allows you to twist, bend and carry a baby, but too much pressure can stretch it out to the point where it separates, like a seam in a shirt. When that gap in your six-pack reaches a distance of 2cm, doctors diagnose diastasis recti.
DR occurs to a lesser degree in men and even infants and young children.
People who get DR outside of pregnancy may do so from repetitive strain in the abdomen, obesity or excessive weight gain, or a connective tissue disorder.
Does Coning Mean You Have Diastasis Recti?
Coning refers to the visual appearance of the belly. You can be coning without having diastasis recti, which is diagnosed at the 2cm separation mark.
The most common method to check for DR is the finger-width method.
- First, lie on your back with your knees bent and feet flat on the floor.
- Lift your shoulders slightly off the ground, keeping one hand behind your head for support. Look down at your belly.
- Move your other hand above your belly button, palms down and fingers toward your toes.
- Use your fingers to feel for a gap between the abs. If you feel a gap of two or more finger widths, reach out to a healthcare provider for formal diagnosis and care.
When Does Coning Begin?
Typically, in the 2nd and 3rd trimesters the abdominal muscles have to separate to make room for the growing baby. This separation can range from just under an inch to about 8” wide. This is when pregnant women are most at risk for coning.
What Does Abdominal Coning Look Like?
Your belly will have a pointy midline running from the breastbone to the belly button during pregnancy. The ridge running down the midline of the abdomen becomes more prominent with straining and may disappear when the abdominal muscles are relaxed.
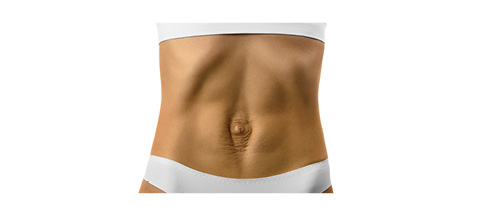
Postpartum coning may look like a separation in the middle of the six-pack, like a gulch. It can also present as a soft protrusion postpartum, pushing the belly button out, sometimes referred to as “mummy tummy” or “mom pooch.”
What Does Abdominal Coning Feel Like?
Abdominal separation itself is not painful, but the side effects can be. These include a feeling of abdominal weakness or lack of core stability, low back pain, pelvic pain, constipation, and incontinence. In severe cases, the thinning of the abdominal wall can lead to a hernia.
What Causes Coning During Pregnancy? Is It Normal?
Coning happens when the uterus starts to push through the abdominal wall with the pressure of the growing fetus. The normal width of the linea alba connecting the abdominal muscles should accommodate carrying a fetus, but sometimes it separates instead, and that’s what causes coning.
It is common during pregnancy, but not everybody gets it. While research is scant for this issue, the common component among those who get it is not fitness but force: the pressure on the abdomen. Women most at risk are those with tight abdominal muscles before pregnancy, carrying large babies or multiple babies, over 35 years of age, petite or short-torsoed, or with a history of C-section, surgery, or weak connective tissues.
Patterns of movement and exercise habits also play a key role [*]. Things that change the pressure in your abdomen — like coughing, pooping, laughing, lifting weight, and giving birth — can, over time, cause DR.
Perhaps the biggest factor is whether you’ve given birth previously. Coning is more commonly seen in women who have had more than one pregnancy — far more common, in fact.
It is estimated that 1 in 3 women (37%) will have abdominal separation after their first pregnancy, and 2 in 3 women (67%) who have had multiple pregnancies will have abdominal separation [*].
How Can I Avoid Coning During Pregnancy?
To avoid widening the separation beyond what is needed for your baby, refrain from doing things that put pressure on these already stretched muscles, such as:
- Arching the low back.
- Crunch activities (abdominal flexion). To get up or lay down, always roll to your side first.
- Core stabilization (planks, down dog, anything on hands and knees, push-ups, pull-ups, double leg lifts, V-sits, and so on).
- Heavy lifting (including other kids).
This is especially true after the first trimester.
DO perform exercises that keep your deep abdominal muscles active (like the transverse abdominis and pelvic floor) but not stressed, like deep breathing or kegels [*]. If you’re concerned about trying to stay fit during your pregnancy, talk to a certified personal trainer or physiotherapist who’s experienced working with expectant mothers.
How Do You Fix an Abdominal Coning?
Post-partum, abdominal separation is typically treated with corrective exercises and strengthening exercises for the muscles that manage intra-abdominal pressure. These exercises are based on the width and the depth of the separation and the patient’s stage in pregnancy or postpartum.
That said, core work done improperly or alone can not only be ineffective, it can make it worse. And studies evaluating the impact of non-specific exercise on preventing or healing DR was inconclusive [*].
Rehab can be effective [*]. A recent study also found neuromuscular electrical stimulation in tandem with strength recovery to be more effective than exercise alone. [*]
In the event rehab doesn't work, a surgeon can fold and sew together the weak central ridge in an abdominoplasty. But keep in mind that surgical repair won’t teach the abdominal muscles to function properly, and for that reason, women who opt to undergo surgery should seek out rehabilitative therapy as well following the surgery. Keep in mind these surgeries can be costly and many insurance companies consider them to be cosmetic procedures and therefore don’t cover them.
That said, if you do opt for surgical intervention, it’s recommended to wait for at least a year after the birth to allow your body to heal and the abdominal muscles to retract [*].
The key takeaway is to focus on exercises that restore function and mobility, not aesthetics, and to consider the big picture as well: the way you carry yourself and your patterns of movement.
Abdominal Coning Postpartum: Does It Go Away? How Long Does It Take?
These muscles will typically come back together within the first few months after delivery, but not always. Research suggests that at least 60% of women have DR six weeks after birth and 30% have it a year after birth, but most women have never heard of it [*].
Complicating matters is the fact that women aren’t routinely screened for DR at the standard postpartum visit around 6 weeks following birth. And if they are, they may be told that core work like crunches will tone the area and close the gap.
Many women only hear about DR in an exercise class or venue outside their doctor’s office.
If you think you have DR, get evaluated by a pelvic health physical therapist or urogynecologist, the professionals who see the condition most.
Left untreated, this underreported condition can lead to pelvic floor dysfunction like incontinence or vaginal prolapse, loss of stability, pain or reduced sensation during sex, and back pain [*].
Some women elect to live with the abdominal separation if it’s not too big and they don’t have pain or complications, but it’s important to bring those muscles back together before you have another pregnancy.
The Bottom Line
Many pregnant women will never experience abdominal coning, and many more will not know what it is or have it properly diagnosed and treated.
Coning is generally not painful during pregnancy but when that separation between the abdominal muscles reaches the 2cm mark it typically indicates diastasis recti, a potentially serious condition with painful and debilitating side effects postpartum.
Unfortunately, there is not a great deal of research on the most effective ways to avoid and treat DR. Those who see the condition most advocate for reducing stress on the abdominal wall muscles during exercise and everyday movement and strengthening the transverse abdominis and muscles of the pelvic floor with exercises prescribed by a professional.
DISCLAIMER: THE INFORMATION ON THIS WEBSITE IS NOT INTENDED TO BE USED AS MEDICAL ADVICE.The materials and information contained on the MiracleCord website is provided for educational and informational purposes only, and is not intended to, and does not constitute, medical or other health advice or diagnosis, and should not be used as such. You should not use this information to diagnose or treat a health problem or disease. If you are seeking personal medical advice, you should consult with a licensed physician. Always consult with a qualified health care provider regarding a medical condition.